As the name implies, fungal skin infections are infections caused on skin by the growth of certain types of fungus. Generally fungi reproduce through tiny spores in the air which sometimes land on our skin. These fungi feed on the protein called keratin which is found in our skin, hair and nails.
Different Types of Fungal Skin Infections
Depending on the type of organism involved, there are four main types of fungal skin infections:
- Dermatophyte infections are those in which fungi affect skin, nail and hair. These are very common and include:
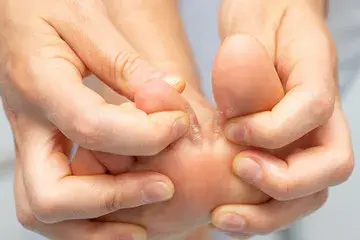
- Athlete's Foot, also known was tinea pedis or ringworm infection of foot. It makes the skin of the foot itchy, dry, scaly and red. There is also a burning sensation along with blisters and sores sometimes. It is very common during warm and humid climates, especially among people who wear tight shoes, have excessively sweating feet and use swimming pools. If hands get contaminated with the affected area, it may spread there too.
- Onychomycosis, also known as tinea unguium i.e. ringworm infection of nails. The nails become thickened, malformed and discoloured.
- Jock Itch, also known as tinea cruris or ringworm infection of groin. It is very common in sportspeople and young men who sweat a lot. An itchy red rash occurs in the groin and surrounding area.
- Tinea corporis or ringworm infection of the body. Abdomen and limbs are the affected areas with red-colored patches either flat patches or elevated rings spreading from centre to outside.
- Tineacapitis or ringworm of the scalp. Very common in young children and cause inflammation of the scalp leading to hair loss.
Also Read: 13 Instant Home Remedies for Burning Feet Sensation Yeast Infections include skin infections caused by yeast and include:
- Thrush is caused by Candida albicans which naturally resides in human body and is usually harmless. But under certain conditions, it multiples excessively and causes ill-effects. The fungus usually grows in moist areas such as skin folds, genitals, under the women's breasts etc. It is characterised by itchy, red-purple patches on the skin with occasional scaling and blisters. Baby with nappy rash are also at risk.
- Intertrigo is also caused by Candida albicans which lives on the skin and in the digestive system. It also affects the same areas as above but is characterized by deposition of white-yellow curd-like fluid on the infected area that itches, sores and is scaly.
- Pityriasis versicolor, also known as tinea versicolor, is characterized by flaky discoloured patches of white or pink color that appear on chest and back. It is caused by yeast of Malassezia species.
Who are at risk of getting fungal skin infections?
Though fungal skin infection can affect anyone but the following categories of people are more vulnerable:
- Those who were recently on antibiotics
- Those who are on steroids
- Those with high blood sugar levels
- Those who are overweight
- Those with weak immune system for example otherwise or due to cancer or HIV/AIDS
- Those who had been infected with it in the past
Don't forget moist skin is welcoming environment for the growth of fungus so keep your skin dry as much as possible, especially after bathing or sweating.
Are fungal skin infections contagious?
Yes, Fungal skin infections are highly contagious and quickly spread from one person to the other. Gyms and swimming pools used by a person infected with fungus acts as a carrier for the disease. Also contact with any personal items of affected person like bed sheet, towels, combs etc. spreads fungal infections. Cats, dogs and cattle also act as the carrier of ringworm infection.
How is the diagnosis done?
The general practitioner will enquire about the symptoms and examine you. He/she will most probably refer you to a dermatologist (or skin specialist). Dermatologist will take a sample of the affected area, skin or scalp scraping, nail or hair fragment as the case may be, and send it for laboratory investigation to confirm the diagnosis.
What is the treatment for fungal skin infections?
Fungal skin infections are usually treated with topical antifungal treatment like creams, lotions, sprays, shampoos and medicated powders. These are to be applied directly on the affected areas. If the infection is widespread, then the doctor may also prescribe some oral antifungal drugs like itraconazole, fluconazole, ketoconazole and terbinafine etc. based on their diagnosis. Also Read: Try Out These Ultimate Foot Care Routine For Magnificent Results
How to prevent fungal skin infections?
It is very difficult to safeguard against prevalent fungal skin infections' spores but here are some 10 simple things that can you can do in your everyday life to reduce the risk of getting fungal skin infections:
- Dry your skin thoroughly after bathing.
- Take a bath if you have sweat heavily
- Wear loose fitting cotton clothes and inner wear, especially during workouts.
- Choose cotton fabric socks and inner garments as compared to synthetic ones. Cotton allows skin to breathe.
- Use your own personal items like combs, towels etc. instead of sharing with others.
- Don't wear same socks and shoes for more than 3-4 days. Give them some time to dry.
- Disinfect pillows, bed sheets and other such items used by someone who has fungal skin infections in the family.
- Wash bed linen and clothes frequently.
- Avoid walking barefoot in public places
- Keep blood sugar levels under check if you are a diabetic.
Also Read: 13 Instant Home Remedies for Burning Feet Sensation

Reviewed by







